Ciprofloxacin (Cipro) is a common antibiotic, but its use can sometimes lead to Clostridium difficile (C. diff) infection. This occurs because Cipro disrupts the natural balance of gut bacteria, allowing C. diff to thrive. Approximately 10% of patients treated with Cipro experience C. difficile-associated diarrhea (CDAD).
Early detection is key. Symptoms of CDAD include watery diarrhea, abdominal cramping, and fever. If you experience these after a course of Cipro, contact your doctor immediately. A stool sample test will confirm a C. diff infection.
Treatment for CDAD varies depending on the severity. Mild cases might only require supportive care, such as increased fluid intake. More severe cases may require specific antibiotics, such as metronidazole or vancomycin. Your physician will determine the most appropriate course of action based on your individual health status.
Prevention is better than cure. Although Cipro is prescribed for various bacterial infections, explore alternative antibiotic options with your doctor whenever possible. Strict adherence to hand hygiene and infection control measures also significantly reduce the risk of contracting C. diff. This includes thorough handwashing and avoiding contact with contaminated surfaces.
- C. diff and Cipro: Understanding the Connection
- How Cipro Increases C. diff Risk
- Protecting Yourself
- Recognizing C. diff Symptoms
- What is C. difficile (C. diff)?
- Symptoms of C. difficile Infection
- Risk Factors
- What is Ciprofloxacin (Cipro)?
- How Ciprofloxacin Disrupts Gut Microbiota
- Mechanisms of Disruption
- Consequences of Imbalance
- Minimizing Disruption
- Long-Term Effects
- The Link Between Cipro Use and C. diff Infection
- Understanding the Mechanism
- Reducing Your Risk
- Further Considerations
- Risk Factors for C. diff Infection After Cipro Use
- Symptoms of C. diff Infection
- Recognizing Serious Symptoms
- Less Common, but Noteworthy Signs
- When to Contact Your Doctor
- Diagnosing C. diff Infection
- Testing Methods
- Further Diagnostic Considerations
- Treatment Options for C. diff Infection
- Preventing C. diff Infection After Cipro Prescription
C. diff and Cipro: Understanding the Connection
Ciprofloxacin (Cipro) is a fluoroquinolone antibiotic frequently prescribed for bacterial infections. However, Cipro use significantly increases your risk of developing a Clostridioides difficile (C. diff) infection. C. diff is a bacterium causing diarrhea and potentially life-threatening colitis.
How Cipro Increases C. diff Risk
Cipro disrupts the natural balance of gut bacteria. This disruption allows C. diff, which is normally kept in check by other gut bacteria, to overgrow. The resulting overgrowth leads to the production of toxins that damage the colon, causing symptoms such as severe diarrhea, abdominal pain, and fever. The severity ranges from mild to life-threatening.
Protecting Yourself
Minimize Cipro use: Discuss alternatives with your doctor. Only take Cipro if absolutely necessary. Hygiene is key: Practice meticulous hand hygiene to minimize the spread of C. diff spores. Antibiotic stewardship: Doctors are encouraged to prescribe antibiotics responsibly, avoiding unnecessary use. Prompt treatment of C. diff: If symptoms arise, seek medical attention immediately. Early treatment improves outcomes. Probiotics: Some studies suggest probiotics may help restore gut flora balance, although more research is needed.
Recognizing C. diff Symptoms
Watch for watery diarrhea (often more than three times a day), abdominal cramping, fever, and loss of appetite. These can indicate a C. diff infection. Contact your doctor immediately if you experience these symptoms, especially if you have recently taken Cipro or other antibiotics.
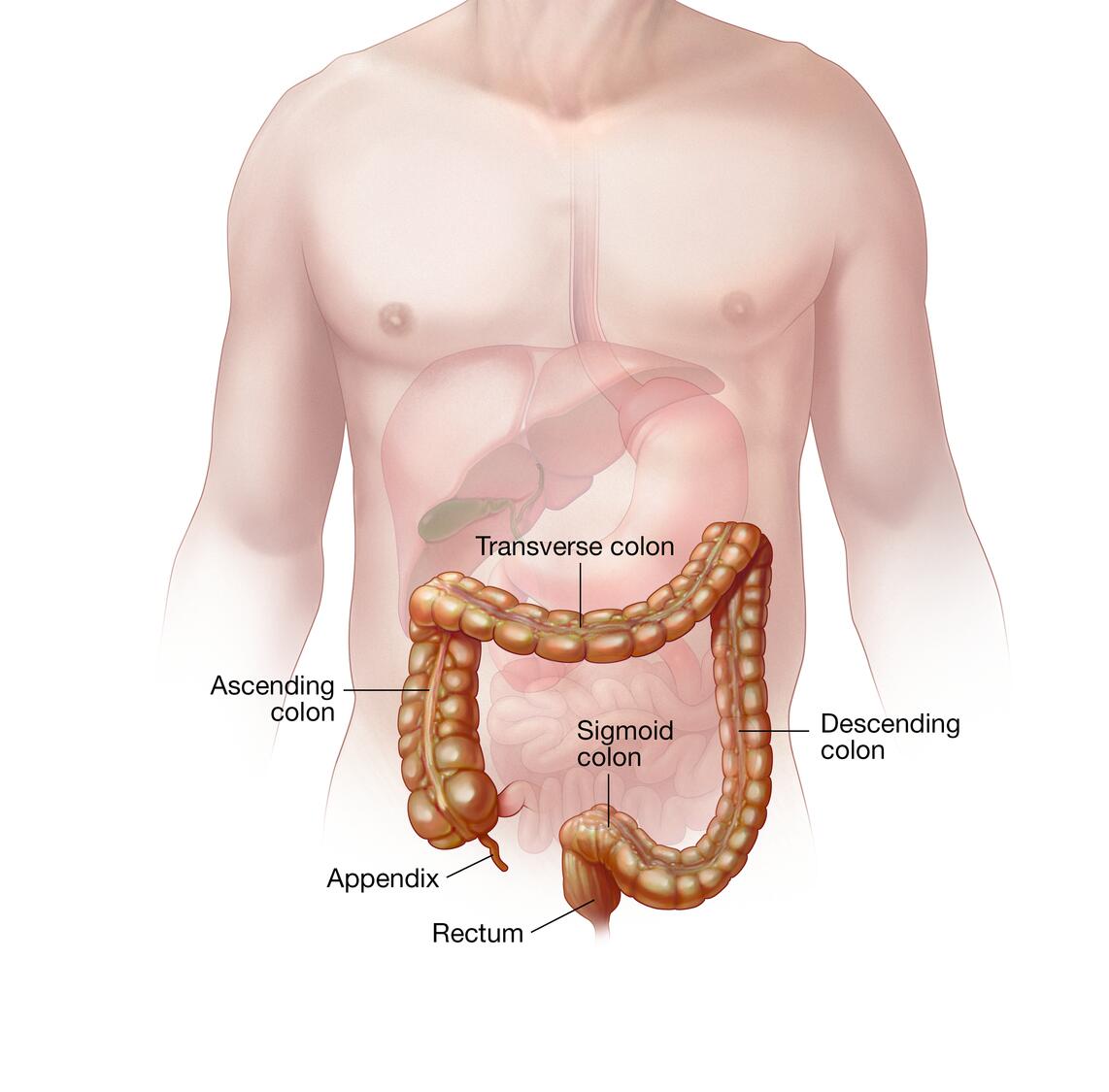
What is C. difficile (C. diff)?
C. difficile, or Clostridioides difficile, is a bacterium causing infection in the intestines. It produces toxins that damage the lining of the colon, leading to diarrhea, fever, and abdominal pain. This infection is most common in people who have recently taken antibiotics, as these medications disrupt the natural balance of gut bacteria, allowing C. diff to flourish.
Symptoms of C. difficile Infection
Symptoms vary but frequently include watery diarrhea (often more than three times a day), abdominal cramping, and fever. Severe cases can lead to colitis (inflammation of the colon), toxic megacolon (severe colon swelling), and even death. Seek immediate medical attention if you experience these symptoms, especially if you’ve recently received antibiotics.
Risk Factors
Advanced age, weakened immune system, and recent antibiotic use significantly increase your risk. Hospitalization and long-term care facilities also present a higher risk of exposure. Proper hand hygiene and infection control practices are key in preventing the spread.
What is Ciprofloxacin (Cipro)?
Ciprofloxacin, commonly known as Cipro, is a powerful antibiotic belonging to the fluoroquinolone class. It targets a broad spectrum of bacteria, effectively treating various infections.
Cipro works by inhibiting an enzyme crucial for bacterial DNA replication and repair. This halts bacterial growth and ultimately kills them. Doctors prescribe it for a range of conditions including urinary tract infections, respiratory infections like pneumonia, and certain types of skin infections.
While generally safe, Cipro can cause side effects. Common ones include nausea, diarrhea, and headache. More serious, though less frequent, side effects involve tendon damage or nerve problems. Always inform your doctor about all medications you are taking, including over-the-counter drugs and supplements, to minimize potential interactions.
Remember, Cipro is a prescription medication. Never take it without a doctor’s prescription or deviate from the prescribed dosage and duration. Self-treating can lead to antibiotic resistance and potentially worsen your condition. Always follow your doctor’s instructions carefully and promptly report any unusual symptoms.
Before starting Cipro, discuss your medical history with your physician, especially if you have a history of seizures, kidney or liver problems, or are pregnant or breastfeeding. Your doctor will help determine if Cipro is the appropriate treatment for you and manage any potential risks.
How Ciprofloxacin Disrupts Gut Microbiota
Ciprofloxacin, a broad-spectrum antibiotic, targets a wide range of bacteria, including beneficial gut flora. This indiscriminate action significantly alters the gut’s microbial composition. Specifically, it reduces bacterial diversity, impacting the delicate balance necessary for proper digestion and immunity.
Mechanisms of Disruption
Ciprofloxacin’s mechanism involves inhibiting bacterial DNA gyrase and topoisomerase IV, enzymes vital for bacterial DNA replication and repair. This process isn’t limited to harmful bacteria; it also affects beneficial gut microbes, leading to a decrease in their populations. This imbalance creates an environment prone to opportunistic infections like C. difficile.
Consequences of Imbalance
The resulting dysbiosis–an imbalance in gut microbiota–can manifest in several ways. Reduced short-chain fatty acid production, crucial for gut health, is a common consequence. This can lead to symptoms like diarrhea, abdominal pain, and impaired nutrient absorption. Furthermore, the weakened gut barrier increases the risk of inflammation and systemic infections.
Minimizing Disruption
Probiotics, containing beneficial bacteria, may help restore gut flora after ciprofloxacin treatment. A diet rich in prebiotics, which feed beneficial bacteria, also supports recovery. Always discuss antibiotic use with a doctor to ensure appropriate usage and to minimize potential adverse effects on the gut microbiome. Remember to always follow your doctor’s instructions regarding medication.
Long-Term Effects
While most individuals recover, some experience persistent gut issues even after ciprofloxacin is discontinued. These lingering effects highlight the significant impact of this antibiotic on the gut’s complex ecosystem. Further research explores the long-term effects and potential preventative strategies.
The Link Between Cipro Use and C. diff Infection
Ciprofloxacin (Cipro), a fluoroquinolone antibiotic, disrupts the balance of your gut bacteria. This imbalance allows Clostridioides difficile (C. diff), a bacterium resistant to many antibiotics, to flourish and cause infection. The risk increases with higher doses and longer treatment durations.
Understanding the Mechanism
Cipro targets a broad range of bacteria, including beneficial gut flora. This disruption weakens your gut’s natural defenses against C. diff spores. These spores then germinate, leading to toxin production and potentially severe illness, including diarrhea, colitis, and even death.
Reducing Your Risk
Probiotics: Consider supplementing with probiotics during and after Cipro treatment to help restore beneficial gut bacteria. Narrow-spectrum antibiotics: Discuss alternatives with your doctor; if possible, choosing a more targeted antibiotic may lessen the risk. Infection control: Meticulous hand hygiene is paramount to prevent the spread of C. diff. Careful monitoring: Closely monitor for symptoms of C. diff infection (watery diarrhea, fever, abdominal pain) and report them immediately to your healthcare provider. Early detection greatly improves outcomes.
Further Considerations
C. diff infections are frequently seen in healthcare settings, making hospital stays a period of increased risk. Your doctor can assess your individual risk factors and determine the best course of action for you.
Risk Factors for C. diff Infection After Cipro Use
Ciprofloxacin, a common antibiotic, disrupts the gut microbiome, increasing your risk of Clostridium difficile (C. diff) infection. Several factors amplify this risk.
| Risk Factor | Explanation |
|---|---|
| Advanced Age | Individuals over 65 have weaker immune systems, making them more susceptible to C. diff. |
| Recent Antibiotic Use | Prior antibiotic use, especially broad-spectrum antibiotics, further weakens gut flora, creating a fertile ground for C. diff. |
| Hospitalization or Healthcare Facility Stay | Exposure to C. diff spores in healthcare settings significantly increases infection risk. |
| Underlying Health Conditions | Conditions like inflammatory bowel disease (IBD) or weakened immunity (from diseases like HIV or cancer treatments) increase vulnerability. |
| Length of Ciprofloxacin Treatment | Longer courses of Ciprofloxacin lead to greater disruption of the gut microbiota, hence a heightened risk. |
| Proton Pump Inhibitor (PPI) Use | Concomitant use of PPIs, which reduce stomach acid, can indirectly increase C. diff risk by altering gut environment. |
Understanding these factors allows for proactive measures. Discuss your individual risk profile with your physician, especially if you have any of these conditions. They can help determine the best antibiotic strategy and ways to mitigate C. diff risk.
Symptoms of C. diff Infection
C. difficile infection symptoms vary, but common signs include diarrhea. This diarrhea is often watery and may be accompanied by fever, stomach cramps, and loss of appetite. The severity ranges from mild to severe.
Recognizing Serious Symptoms
Seek immediate medical attention if you experience:
- Diarrhea for more than three days
- Severe abdominal pain
- Bloody diarrhea
- High fever (over 102°F or 39°C)
- Significant dehydration (dry mouth, dizziness, decreased urination)
Less Common, but Noteworthy Signs
While less frequent, these symptoms may also indicate a C. diff infection:
- Nausea
- Vomiting
- Weight loss
When to Contact Your Doctor
Don’t hesitate to contact your healthcare provider if you experience persistent diarrhea or any of the symptoms listed above. Early diagnosis and treatment significantly improve outcomes.
Diagnosing C. diff Infection
Doctors diagnose Clostridioides difficile (C. diff) infection primarily through stool testing. This involves a stool sample sent to a lab for analysis. The lab will check for the presence of C. diff toxins, which are substances produced by the bacteria that cause the damaging effects on the intestines. A positive result confirms the infection. A negative result doesn’t always rule out C. diff, however, as some tests may miss low levels of toxin.
Testing Methods
Several lab tests exist to detect C. diff. These include enzyme immunoassays (EIAs) which look for the toxins, and nucleic acid amplification tests (NAATs) which detect the bacteria’s genetic material. NAATs are generally more sensitive than EIAs, meaning they’re better at detecting even small amounts of the bacteria. Your doctor will determine the best test based on your symptoms and medical history. Sometimes, additional tests are needed to rule out other potential causes of your symptoms.
Further Diagnostic Considerations
Colonoscopy, while not routinely used, may be considered in complex cases. It allows direct visualization of the colon and can reveal the extent of the damage caused by C. diff. Imaging tests like abdominal X-rays or CT scans aren’t used to diagnose C. diff itself, but can help assess the severity of the complications like colitis or megacolon.
Treatment Options for C. diff Infection
Treatment for Clostridioides difficile (C. diff) infection focuses on eliminating the bacteria and supporting your recovery. The most common treatment involves antibiotics.
- Metronidazole: This is often the first-line treatment for mild to moderate C. diff infections. Expect to take it orally for 10-14 days.
- Vancomycin: This is a stronger antibiotic, usually reserved for more severe infections or those that haven’t responded to metronidazole. Oral vancomycin is typically administered for 10-14 days.
Fidaxomicin is another antibiotic option, often preferred for its reduced risk of recurrence. It’s administered orally, also for 10 days.
Beyond antibiotics, supportive care is crucial. This includes:
- Fluid management: Addressing dehydration resulting from diarrhea is paramount. This may involve intravenous fluids in severe cases.
- Electrolyte correction: Diarrhea can lead to electrolyte imbalances. Your doctor will monitor and correct these as needed.
- Nutritional support: Maintaining adequate nutrition is important for recovery. This might involve a modified diet or nutritional supplements.
For recurrent C. diff infections, treatment strategies become more complex. Options include longer courses of vancomycin, tapered vancomycin, or fidaxomicin. In some cases, fecal microbiota transplantation (FMT) may be considered. FMT involves transferring stool from a healthy donor to the patient’s gut to restore a healthy gut microbiome. This is a highly effective treatment option for recurrent infections but requires careful selection and monitoring.
Always follow your doctor’s instructions precisely regarding medication dosage and duration. Open communication with your healthcare provider is key throughout your treatment. They can tailor your care based on your specific situation and response to therapy. Regular follow-up appointments help track your progress and address any emerging concerns.
Preventing C. diff Infection After Cipro Prescription
Maintain meticulous hand hygiene. Wash your hands thoroughly with soap and water for at least 20 seconds, especially after using the restroom and before eating.
Avoid unnecessary antibiotic use. Ciprofloxacin disrupts your gut microbiome, increasing C. diff risk. Discuss alternatives with your doctor if possible.
Focus on gut health. Incorporate probiotics into your diet through yogurt with live cultures or probiotic supplements. A balanced diet rich in fiber also supports a healthy gut.
Practice safe food handling. Thoroughly cook all meats and wash fruits and vegetables to minimize exposure to harmful bacteria.
Stay hydrated. Adequate fluid intake aids digestion and helps flush out toxins.
| Symptom | Action |
|---|---|
| Watery diarrhea, fever, abdominal cramps | Contact your doctor immediately. These could be signs of a C. diff infection. |
Follow your doctor’s instructions carefully. Complete the entire course of Cipro as prescribed, even if you feel better. Early discontinuation can increase resistance and infection risk.
Keep your living space clean. Regular cleaning and disinfection of frequently touched surfaces, especially in the bathroom, minimizes the spread of bacteria.